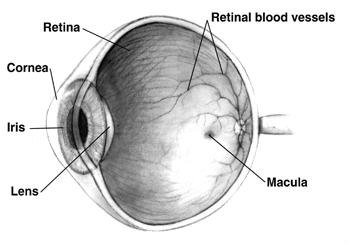
Sight is a complicated process. The simultaneous interaction between many components in the eye creates the detailed and colorful perspective through which we see the world.
Damage to any part of the eye can cause vision loss or impairment, either temporary or permanent.
The Function Of The Macula
Located at the back of the eye, the macula is responsible for our most detailed sight, providing the visual acuity needed to drive cars, read books, and recognize faces. However, the development of macular holes – not be confused with macular degeneration, a separate condition – can blur or otherwise distort a person’s vision, making it difficult or impossible to perform many of these day-to-day activities.
Causes Of Macular Holes
The development of macular holes, small tears in the macula of the eye, is most commonly associated with the aging process, especially in individuals over the age of sixty. Women and people who have previously had macular holes are also more likely to develop them. Holes can occur for a variety of reason, including:
- Shrinking and/or separation of the gel-like material known as the vitreous humor that fills the space between the retina and the lens
- Eye diseases related to diabetes
- Moderate to severe degrees of myopia (nearsightedness)
- Macular pucker, the presence of scar tissue on the macula
- Detached retinas
- Best’s disease, an inherited condition that causes cysts to grow on the macula
- Injury to the eye
The Effects Of Macular Holes
When a macular hole develops, vision loss can be gradual or immediate, depending on the location and size of the tear. Symptoms of macular holes include:
- poor detailed vision at any distance
- distorted, wavy, or foggy vision
- dark or blind spots in the center of vision.
Examples of how macular holes can distort your vision.
Because the macula only affects our straight-ahead vision, macular holes will not affect a person’s peripheral (side) vision.
If you have any of these symptoms, consult your eye doctor.
Testing
Ophthalmologists have a variety of methods to test for macular holes. The first step is a visual exam in which the eye doctor dilates the pupil and then uses a light to examine the retina. If needed, he or she may then perform a fluorescein angiography in order to dye and illuminate specific areas of the eye.
For very small holes that may be otherwise undetectable, an ophthalmologist may need to conduct a more complicated procedure, called an optical coherence tomography. During an OCT, a laser is used to scan and photograph the patient’s retina in order to measure the amount and thickness of vitreous fluid in the eye, as well as any swelling that might be occurring.
In addition to diagnosing the existence of a macular hole, ophthalmologists must also determine its severity. Macular holes develop in three stages, each with increasing vision loss.
Stage I is a detachment of the fovea, a small area in the macula. If untreated, approximately half of all foveal detachments will progress to
Stage II, partial-thickness holes, or
Stage III, full-thickness holes.
Nearly 70% of all Stage II and almost all Stage III macular holes worsen without treatment.
Treatment
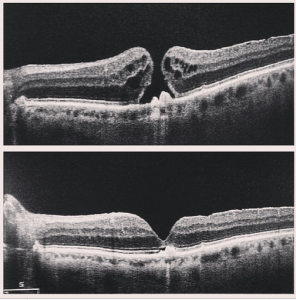
Surgical repair of macular hole on OCT
Because they are rarely self-healing, macular holes should be treated as soon as possible to avoid further vision loss. A vitrectomy is the most common treatment for macular holes. During this procedure, the vitreous gel from inside the eye is removed and a mixture of air and gas is inserted into the now-empty space between the retina and the lens. A bubble then forms and “pushes” on the edges of the hole in order to encourage healing.
However, this procedure has its share of drawbacks. Unlike LASIK, or other laser eye surgeries, vision restoration from a vitrectomy occurs gradually over time as the tear heals. Depending on the size and severity of the macular hole, the recovery time from a vitrectomy can be as long as three weeks. And, in order to keep the bubble in place, patients must lay face-down the entire time. Cataracts, infection, and detached retinas are also possible complications, but they are treatable.
Additionally, patients who undergo a vitrectomy cannot travel by air for several months after the surgery. The changes in air pressure during the flight will cause the bubble to expand and change shape, possibly causing vision damage. Once healed, the patient’s ophthalmologist will remove the bubble or it will dissolve on its own.
A century ago, macular holes were untreatable, leaving those who developed tears in their macula to slowly watch their vision blur and fade away over time. Now, with advances in medical knowledge and technology, we have the ability to see with detailed, colorful vision well into our golden years. If you’ve noticed deteriorating vision, meet with your eye care specialist to discuss these and other options.